Being a mum or dad to a baby on the neonatal intensive care unit (NICU) is incredibly tough on your mental health. Instead of cribs and mobiles there are wires and machines. Instead of introducing a new baby to joyful friends and family, there are hours of sitting, helpless and anxious beside an incubator not knowing if you’ll ever get to take your baby home.
That’s why, as part of the Tiny Lives Appeal, you have helped us to fund an emotional support service for NICU families. Here, five mums tell us their stories and demonstrate why professional emotional support is so vital along the journey.
Michelle – Eden-Olive’s mum

My name is Michelle Gee. I am 34 years old. On September 12th 2017 at 8:04 pm I gave birth to my first child by emergency c section.
Eden-Olive was born 5 weeks prematurely with rare birth defects – oesophageal atresia and trachea oesophageal fistula. Eden-Olive was taken straight to neonatal intensive care. I did not see my baby until the next day at around 11am. I felt my baby had been taken from me. I felt completely empty.
When Eden-Olive was two days old, they took her for life saving surgery. We were prepared for what may go wrong and told we could lose her and then we were handed a consent form to sign. Can you even imagine how it feels to sign a form to say you understand that your baby may die? A nurse then insisted the porters and doctors hold off for five minutes so that we could hold our baby for the first time. We were completely aware why he was doing this – because there was a chance we’d lose her.
Our daughter was in theatre for what felt like forever. Her surgery was a success but when they brought Eden back from surgery it was the most frightening thing I had ever seen in my life. Tubes everywhere; a tiny swollen baby – paralysed and sedated. Although Eden’s surgery was a success and they had managed to repair her oesophagus, she was left unable to feed.
At around two weeks we put Eden to my breast. She was amazing. She knew what to do and both Eden and I took to it just perfectly. But within a few minutes my baby turned blue and floppy in my lap and she had to be revived. This happened more times that I can recall. I remember feeling like every time this happened my baby looked like she’d gone on my lap. I used to scream when it happened. This has left me so traumatised that at times I would shake while holding her.
Eden wasn’t allowed to oral feed after this. The pain of knowing she could feed and wanted to but couldn’t was completely heart breaking. I expressed milk every 2.5 hours for three months knowing Eden was not getting much of my milk. This really effects your mind. I became obsessed with making milk for my baby. Longing to breast or bottle feed her – to just do the most natural things and give her nutrients.
My baby spent her first 11 months in hospital. She spent the first four and a half on the neonatal unit and was then transferred to Island ward at the children’s hospital.
Since being born, Eden has endured countless intensive painful procedures, caught I don’t know how many viruses, been on life support five times and had two major surgeries. Our baby has lots of blue episodes where she chokes and her airway collapse. This doesn’t get any easier, it’s still as scary as the first time.
Some days I felt like I was losing my mind but how could I do that when I needed to be the best mother I can be? I never left the hospital so getting support was hard.
The nursing staff and doctors on the neonatal unit are amazing but they are there to take care of their patients and you can’t expect them to counsel families while doing such an important job like caring for sick babies.
Rachel – Jake’s mum
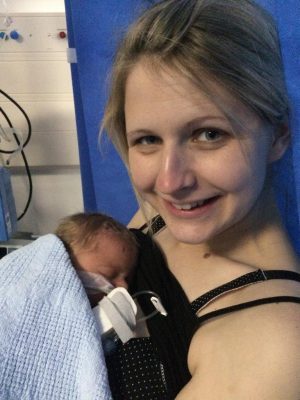
The impact of going into hospital heavily pregnant and coming home without a baby is really traumatic. I and other mums I know used to wake in a sweat desperately trying to remember what has happened and sometimes searching the bed for the baby in a half asleep state. I couldn’t bring myself to tell many close family the extent of Jake’s illness and had to ask my mum to call many people as nothing can prepare you for finding the words to tell your family that their first grandchild/ niece /nephew is unlikely to survive. Registering your new baby’s birth while they lay fighting for their lives, the first time you say out loud “I am Jake’s mum” into the NICU video entry system- all really hard things to come to terms with.
The experience of having a critically ill baby is never going to be easy. But the care and attention of the amazing staff in the NICU make every step of the process easier. Knowing your baby is in the safest hands makes the sleepless nights more bearable. The generosity of those giving to the Tiny Lives Appeal has already meant that babies can have the best start in the best environment. To be able to add psychological support for parents to this would mean that both babies and parents are given the best possible chance to come out the other side of their experience with the best chance of moving forward.
Nicola Madoc-Jones – Edie’s mum

My daughter was born at 23 weeks gestation. My pregnancy was healthy, my baby was thriving and everything was going as it should, but just two and a half weeks after my 20 week scan, I found myself 2cm dilated and admitted to the delivery suite at the University Hospital Wales. Just like that.
Three days later my daughter was born. During our three day hospital stay prior to her birth, we were dealt with one blow after another. They didn’t know whether her birth was imminent or not, we just had to wait and see. Not knowing and the having to wait and see, alone, is enough to truly damage your mind. The feeling of helplessness is unbearable. But when hearing that if your healthy baby will be considered a miscarriage if she arrives before 24 weeks, well that is just soul destroying.
We were provided with dire statistics. Only 20% of 23 weekers will survive and 50% of those that do will have moderate to severe disabilities. After being provided with such devastating statistics, we were asked to make a decision about whether we wanted doctors to resuscitate our baby at birth. How were we supposed to make a decision like that when we loved our unborn child like we did and carry that type of weight without being mentally scarred afterwards?
During my labour, my baby’s heartbeat was good. We know because the midwives suggested that we film it. But we knew only too well, even then, why they did that – because they assumed that she would die and that it would be all we’d have left. Her heart rate was fine until my waters broke. Suddenly finding herself not in the water, she began to deteriorate rapidly. Her heart rate dropped to 50 beats per minute. I knew I had to deliver her quickly because if born without a heartbeat, she wouldn’t receive medical assistance.
Edie was born severely bruised from the delivery and the sight of her was shocking. At 580 grams (1lb 4oz) she was the smallest thing I had ever seen. Numerous doctors and nurses quietly worked on her and it seemed to take a lifetime. We didn’t know whether they were going to turn around and say that the resuscitation was successful or not but eventually she was ventilated and put in the transport incubator. They wheeled her to the bottom of my bed and as they started to take her away, the doctor turned to me and said, “the odds are not good.” I couldn’t see her for another four hours and in that time we didn’t know if we’d be seeing our baby alive or dead.
For me, going from complete happiness and normality to being thrown into this hellish situation with no prior warning was the hardest part. I didn’t have time to think or to deal, I just found myself in it. And it didn’t stop there either.
I remember looking around the NICU for the first time. These were the smallest babies I’d ever seen – until I saw my own baby – the smallest of all. I couldn’t see how someone so small and so premature could ever survive. We’d been given the statistics before Edie had even been born so we started off our journey already programmed into thinking that she would die.
NICU is hard enough but when you start off knowing that statistically, your child is unlikely to survive, it’s hell. Every day I’d wake and think, “Well it wasn’t yesterday, so it must be today.” To have to get dressed and physically take yourself to a place where your baby would likely live her last day, was so difficult. I can’t even describe the pain you feel.
We watched Edie suffer through a brain bleed, numerous infections, multiple blood transfusions, sepsis, chronic lung disease, a collapsed lung, a hole in the heart, retinopathy of prematurity and frequent resuscitation. All of this at 580 grams and all at the same time. At two weeks old, doctors took us into the quiet room and informed us that they were considering turning off Edie’s life support – the worst day of my life. I had never felt such pain before. And I’ll never forget the conversation for as long as I live.
As well as our own situation we experienced the passing of other babies on the unit, both premature and full term. The cries of the fathers and kind words of mothers to their dying babies is something that will haunt me forever. The mixed emotions that come with witnessing such grief is crippling. There’s the incredible sadness and anger at seeing a baby die but also the relief that it wasn’t you, not this time at least. That sense of relief leaves with you with permanent scar of guilt that I carry to this day.
I genuinely don’t think that the human brain is equipped to deal with such extreme emotions. There are so many ups and downs along the NICU journey and some of them can take you by complete surprise. Although in many ways I couldn’t wait to go home with Edie when she was finally well enough, I still felt very sad to be leaving the people who we’d spent every day for four months with, who we had deeply bonded with. They are the people who had nursed our daughter back from near death, who had celebrated her milestones in a way that can only be celebrated by people who saw how close we came to losing her. For the first four and a half months of her life, the NICU was the only place that we had ever physically been with her. It had become our home.
I feel very proud to be involved in an appeal that will help provide a professional emotional support service for NICU parents. I think it will make such a difference.
Laura- George’s mum

On the 16th of July 2016, six days before my planned C Section I woke concerned that my baby had not kicked me through the night. At the hospital I was told that my baby was in fetal distressed and whisked to the operating theatre. My husband made it by the skin of his teeth.
George was born at 17.17 weighing 7lbs 8oz in a good condition. However, at 15 minutes old he crashed in my husband’s arms and required resuscitation in the delivery room. George was rushed to the Neonatal Intensive Care Unit (NICU) and because I was unwell myself I didn’t seem him again until he was two days old. We were told that George was in dire straits, was on life support and that they were doing all that they could for him.
George was being treated for Hypoxic Ischemic Encephalopathy (HIE), a condition caused by a lack of oxygen that can cause brain damage. The treatment involved therapeutic hypothermia where George was cooled for 72 hours and then warmed back up again. This process is a clever medical method that prevents and reverses damage caused to organs by lack of oxygen but it was very frightening. We then had to wait an even more frightening 21 days to confirm that he did not have brain damage. His organs had also avoided any long term damage but his gut and liver had taken a bit of a hit.
During this time we were both diagnosed with sepsis. George was extremely unwell and I had to wait a painful and long 9 days before being able to hold him. I felt helpless and went through a significant grieving process. After 15 days as an inpatient myself I was discharged. Going home without my baby was the hardest thing I’ve ever had to do and I didn’t want people to see me without my baby as it wasn’t meant to be that way. I longed to do ‘normal’ things families do; sit on the sofa with my baby, wake up next to my baby (I’d never spent a night with him), take my baby for a walk in his pram, the list was endless. Instead my days were spent going back and forth the hospital sat next to George strapped to equipment that would beep continuously. Babies would be admitted almost every day but many would come and go. It felt like we were never going to get George home.
George’s blood pressure dropped dangerously and he required cardiovascular support. He was also severely anaemic and had 12 blood transfusions while we were there. His bloods remained deranged with poor liver function as his body triggered an autoimmune response to the infection and he suffered various meningitis type aggressive rashes. He was being seen by specialists from immunology, haematology, dermatology, cardiology, endocrinology and more.
George was tested for a variety of conditions in order to check that nothing was being missed and for a long time we didn’t know if we were facing a significant diagnosis. He underwent 3 lumbar punctures and over 100 blood tests. Fortunately, his bone marrow and all other tests came back normal and immunology and haematology advised that we were to sit patiently and see what happened next. George suffered some complications from the cooling process including a rare skin condition called subcutaneous fat necrosis and hypercalcemia.
George’s condition gradually began to improve and by the 27th of September 2016 he was well enough to go home. But by December I had reached an extreme low. I’d been so wrapped up in my son’s journey that it wasn’t until we left the confines of the NICU that it all hit me. I was tearful, anxious, suffered flashbacks, would cry uncontrollably, I couldn’t sleep properly and I couldn’t bring myself to be around pregnant women or newborn babies because it made me think about where we were at that stage. I felt hyper sensitive and as though I wasn’t a nice person as a result of how I was feeling. I felt alone and like no one understood our start to family life. I actually found myself wishing we were back on the NICU where professionals could understand the importance of small milestones and protect my baby more than I could.
Eventually I got professional support and I can safely say it saved me. Even now two years later something can trigger a NICU memory and it leaves me feeling teary and blue for a few days but the support I received gave me the tools to know how to deal with it. Emotional support is so important for NICU parents because the journey is so unique. Grieving a baby you have not lost is hard for anyone to understand.
George is now a healthy happy two-year-old who’s bursting with life. Every day I’m amazed at how incredible he is and we’ll never be able to repay the doctors, consultants, nurses and support staff on NICU who helped save his life and supported us through such a rollercoaster of a ride. We miss the team daily. After 73 days they really do feel like family.
Lisa Reynolds – Rea’s mum
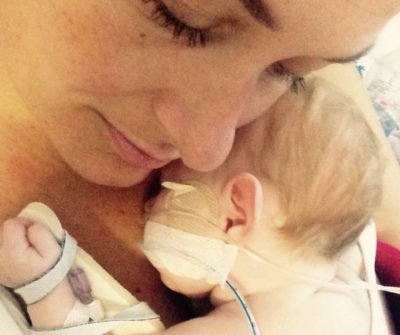
I never thought I’d need professional emotional support. I’m a very open person so I find it easy to talk to friends, family and loved ones.
For the nine months that Rea spent in hospital I talked through things with many people, I cried to everyone, I moaned to anyone who would listen and I relied on my nearest and dearest to get me through it.
When the time came for me to return to work I knew I wasn’t up to it. Aside from the fact Rea was still in hospital, I was an emotional mess, completely drained and actually feared being a teacher again!
I was offered professional emotional support through my employer and although hesitant at first it was the BEST thing I ever did! I really wish I’d been able to access that sooner though because it was such a valuable experience.
Although I felt like everyone around me was always counselling me on some level it wasn’t until I sat with a qualified person that I started to accept some of the things that had happened. She then gave me the coping mechanisms to start to move on from it all. I often wonder if I would’ve been or could’ve been mentally stronger if I’d had that sooner but I guess I’ll never know!
Nobody can ever prepare you for the feelings you will have as a NICU Mummy. And little did I know that these feelings don’t just go away when your baby gets to come home. , I really wish that there was someone to talk to in the early days, on the toughest of days, when nobody else understood what I was going through. I will forever be grateful to everyone who has supported me for the last two years but I’m so pleased that through the Tiny Lives Appeal, future NICU parents will be able to access the professional support they need in the early days.







