
Life on the neonatal intensive care unit can be very fast paced. The condition of the babies cared for there often changes rapidly, from relatively stable to life-threatening, in a matter of seconds. The incredible NICU team is skilled in responding quickly in these situations but to do that, it’s essential that they have the right equipment to hand.
In 2018, Noah’s Ark Charity supporters helped fund state-of-the-art ventilators for NICU that administer all levels of respiratory support to premature and critically ill babies- from the highest to the most minimal. Most vitally, the ventilators allow the medical team to respond rapidly in an emergency, but they also mean that vulnerable babies no longer need to be removed from one machine and re-attached to another. This reduces risk and the chance of infection while also minimising stress, allowing these tiny babies to conserve the vital energy they need to grow and gain strength.
Without the support of a specialised ventilator like this, baby Olwen would not have survived.
Olwen’s story
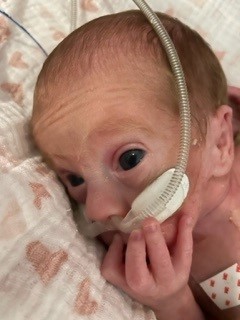 Bethan and Dan knew there was a chance that their first baby would come a little early as Bethan had been diagnosed with low levels of a protein called PAPP-A, which can result in pre-term birth. What the couple didn’t expect was to leave home for a routine check at 28 weeks and not return.
Bethan and Dan knew there was a chance that their first baby would come a little early as Bethan had been diagnosed with low levels of a protein called PAPP-A, which can result in pre-term birth. What the couple didn’t expect was to leave home for a routine check at 28 weeks and not return.
During their routine check-up, the medical team noticed an issue with blood flow through the baby’s umbilical cord.
Bethan was admitted for further monitoring and given steroids to mature the baby’s lungs in case an emergency delivery became necessary. Things improved a little for a while, but a scan three days later showed that the blood flow was now starting to reverse. As a result, a decision was made to deliver the baby that same day. Bethan and Dan were in shock.
Bethan says: “I started crying and couldn’t stop. I was terrified because I’d never even heard of a baby being born that small, yet alone surviving. I was frightened and apprehensive about what she would look like and terrified about what lay ahead.
“I was amazed when I saw her for the first time – looking like a real baby! Her eyes were open, and she even cried. Dan cut the cord and they brought her over so I could see her for a few short minutes before she was whisked away to intensive care. It was another six hours before I was able to go and see her again and to begin with, I felt completely overwhelmed. There were noisy machines everywhere and she looked so small and vulnerable in the middle of it all. I’d get upset every time I walked in during those first few days. Not being able to hold my baby went against every instinct I had.”
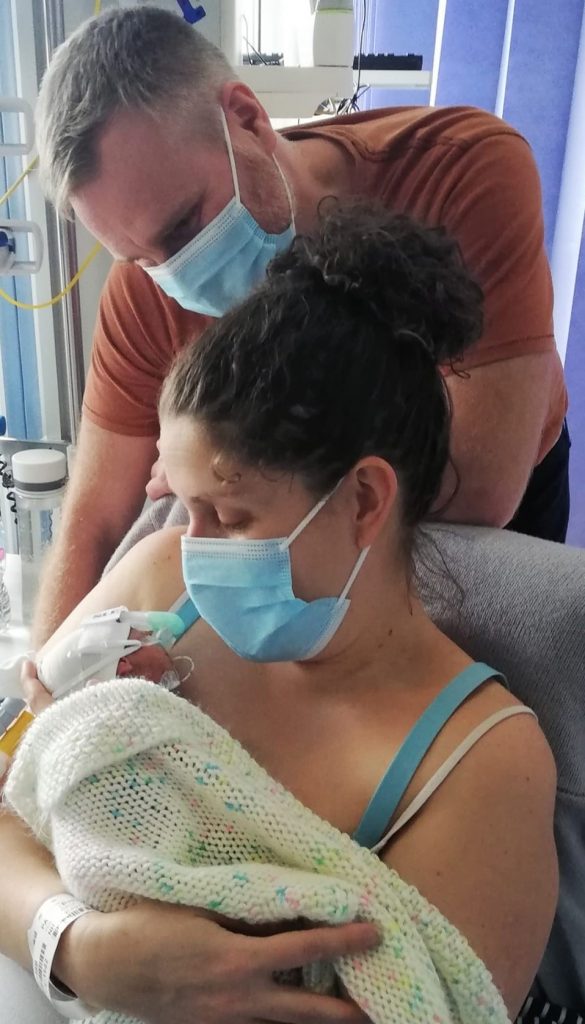 Despite Olwen’s early birth, she did very well at first, only needing a non-invasive type of breathing support called CPAP. But at seven days old, Olwen started to struggle, and her oxygen needs were increased. Suspecting a collapsed lung, her medical team inserted a chest drain but Olwen’s condition continued to deteriorate, and the decision was made to intubate her for full breathing support. Mercifully, thanks to the adaptable ventilator Olwen was on, the medical team was able to respond quickly. By the time Bethan and Dan arrived after a call to come in in the early hours, she was stable.
Despite Olwen’s early birth, she did very well at first, only needing a non-invasive type of breathing support called CPAP. But at seven days old, Olwen started to struggle, and her oxygen needs were increased. Suspecting a collapsed lung, her medical team inserted a chest drain but Olwen’s condition continued to deteriorate, and the decision was made to intubate her for full breathing support. Mercifully, thanks to the adaptable ventilator Olwen was on, the medical team was able to respond quickly. By the time Bethan and Dan arrived after a call to come in in the early hours, she was stable.
Though often vital for survival, full ventilation, often referred to as ‘invasive ventilation’, can result in long-term damage to the lungs if used for a prolonged period. It’s important therefore that a patient is weaned down to a lower type of breathing support as quickly as possible. By the following day, with Olwen showing signs of recovery, the breathing tube was removed, and she was put on a less invasive type of continuous air pressure ventilation called BiPap. But, only a few short hours later, Olwen started to struggle.
Bethan said: “She started to make noises that we hadn’t heard before and her colour started to change. We hadn’t been there when she’d crashed before so when it happened this time, we thought that we were losing her. Suddenly the incubator was surrounded by nurses and doctors and we were told to leave while they re-intubated her. It was the scariest ten minutes of my life!”
After a bumpy week, Olwen seemed to sense for herself that she was on the mend and pulled out the breathing tube herself.
From that point, Olwen went from strength to strength. She graduated through several types of reduced breathing support and moved from intensive care to high dependency and then to the nursery in only a little more than a week.
 In the nursery, Olwen’s main task was to learn how to feed independently so that she could grow and go home. The process took a little longer than hoped but at the end of July, Olwen finally left hospital, assisted only by a small amount of oxygen. She’s now 6lb 12oz and it’s hoped that the bigger she gets the stronger her lungs will become.
In the nursery, Olwen’s main task was to learn how to feed independently so that she could grow and go home. The process took a little longer than hoped but at the end of July, Olwen finally left hospital, assisted only by a small amount of oxygen. She’s now 6lb 12oz and it’s hoped that the bigger she gets the stronger her lungs will become.
Bethan says: “Olwen’s story is a real-life example of how a premature baby’s condition can change rapidly. Several times she went from fine to dangerously unwell in a matter of minutes. Had the clinical team not been able to respond quickly with the right equipment, I don’t want to even imagine how different things might have been. It’s thanks to the specialist care and that specialist equipment that we now have our daughter home with us and we can start living the family life that we’d dreamt of for so long.”
The Noah’s Ark Charity has recently re-launched it’s Tiny Lives Appeal in a bid to raise £300,000 to fund incubators, ventilators and transport incubators for the ever evolving neonatal intensive care unit.








