
The Williams family know a lot about life on the neonatal intensive care unit. Rebekah and Anthony’s first daughter, Anwen, spent 10 weeks on the neonatal intensive care unit (NICU) five years ago after being born 12 weeks early. This year, the couple spent 159 days there after the birth of their twin daughters at just 24 weeks.
When Rebekah became pregnant with twins, the couple were naturally concerned that their babies would be premature. But they were reassured and told, as Anwen’s early birth had most probably been caused by an infection, it was unlikely to happen again.
But Rebekah and Anthony were right to be concerned. Though a check at 17 weeks indicated that everything was fine, a scan three weeks later revealed that Rebekah’s cervix had shortened significantly, meaning that she could go into labour at any time. Being born at only 20 weeks would give the babies zero chance of survival but there was very little anyone could do to stop it, or even predict when it might happen. Terrified, Rebekah was put on bed rest and sent home.
At 24 weeks plus two days, Rebekah went into labour, at which point there was still a very real a chance that her twins would not survive. Thankfully, as there had been prior warning, everything had been done to prepare for the babies’ births, including administering magnesium for their brains and steroids for their lungs. Mali shot out when Rebekah’s waters broke weighing just 620 grams and was whisked away to NICU in a transport incubator. Cari followed soon after at a smaller 591 grams.
Rebekah said: “Having been NICU parents before, we were prepared for that first bit in some ways. Walking onto the unit for the very first time is terrifying but we recognised a lot of the staff there and we knew what all the scary looking machines did. But seeing our tiny babies for the first time was still somehow a shock. We were told that the first few days were critical, that we were at the beginning of a long journey and that things would likely get a lot worse after an initial honeymoon period. The anticipation of that was terrifying.”
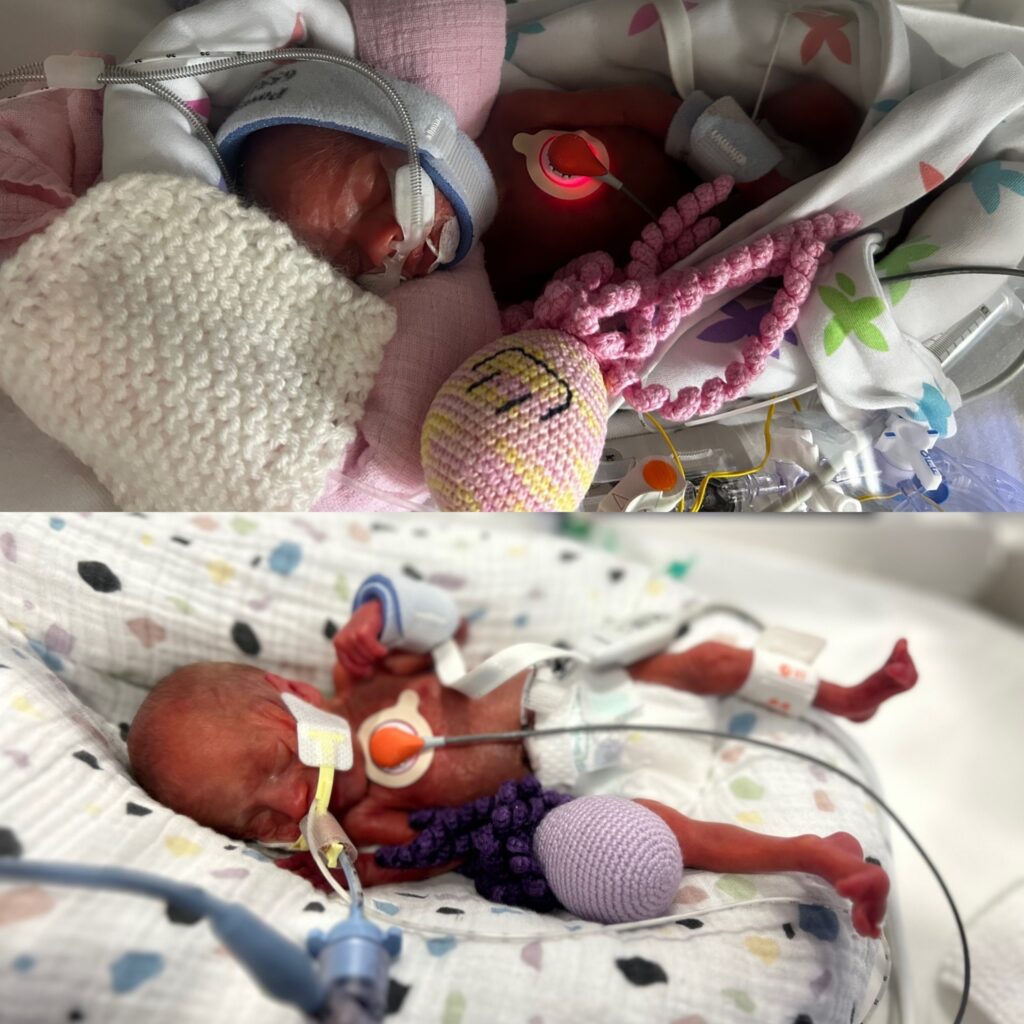
During those first few weeks Mali and Cari came off the ventilators only to have to go back on them again. They had countless blood transfusions, were diagnosed with holes in their hearts and were treated for multiple infections. The twins also had regular head scans, which were particularly frightening for Rebekah and Anthony as their daughter Anwen had been diagnosed with cerebral palsy from a head scan at three weeks old.
Then, at 18 days old, Mali’s condition deteriorated rapidly. She became septic with MRSA had developed a large blood clot that was impacting on both her heart and kidneys. Her body started to swell to the point that she was almost unrecognisable. She was put on multiple antibiotics and had to have a chest drain inserted to remove the fluid from her lungs.
Rebekah says: “Anyone who’s spent time on NICU may be aware of the ‘bad news room’ so when we were taken there on the 26th day, we were prepared for the worst. On top of the sepsis and blood clot, one of Mali’s kidneys had become enlarged and she had stopping weeing. We feared that this was a sign that her body was shutting down. We were told in the kindest way possible to prepare for the worst. I felt so overwhelmingly helpless. None of this was the babies’ fault but they were the ones who were suffering. We’d almost felt at first that because they were in the best place possible that they would be ok. But we’d already experienced two losses on the ward this time and we knew now only too well that it could happen to us too. We went home that night to Anwen, waiting by the phone but willing with all our hearts for it not to ring.”
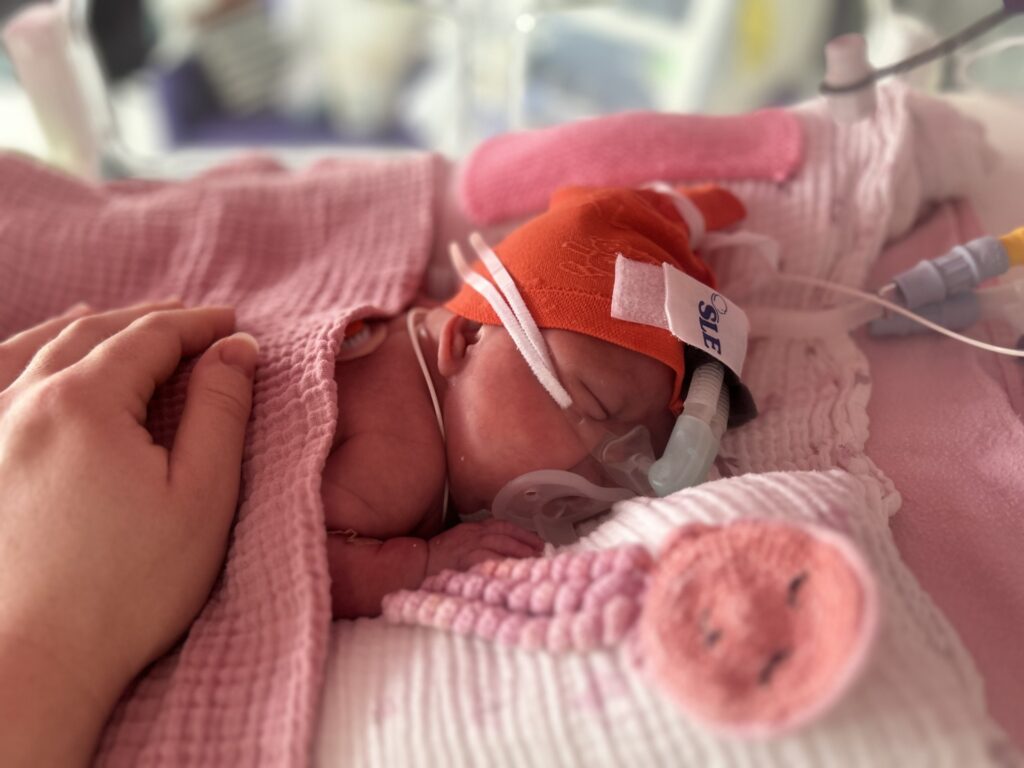
Over the next 48 hours, as her parents tried to face the fact that they may leave without one of their daughters, Mali showed no sign of improvement. Then, on the Saturday evening, a small miracle happened – Mali did a wee! It was a sign that her kidneys were starting to recover and that she was back from the brink!
From then on, Mali and Cari’s progress was slow but steady. By mid-August, both babies were well enough to come off their ventilators and by the end of the same month they had graduated to the High Dependency Unit. The babies still battled with repeated bouts of MRSA, but their main challenge now was to feed and grow.

After 159 long days in NICU, Rebekah and Anthony were able to take their precious girls home. Rebekah says: “We’re not leaving the NICU unscathed, and we know that we’ll rely on the children’s hospital for support for many years to come. We feel so lucky to have the opportunity to take them home but we also know that it isn’t just luck. Mali and Cari’s survival would just not have been in any way possible without the neonatal intensive care unit and its wonderful team. The equipment around them kept them alive – from the incubators that gave them the environment they needed to grow to the ventilators that literally breathed on their behalf for more than two months.”
Right now, the Noah’s Ark Charity is running an appeal to raise £300,000 for the neonatal intensive care unit. Funds raised from the Tiny Lives Appeal will provide transport incubators, ventilators and incubators, all pieces of equipment that are vital in providing care to around 600 of the smallest and sickest babies in Wales each year.








