Joe, Sam and Ollie’s story
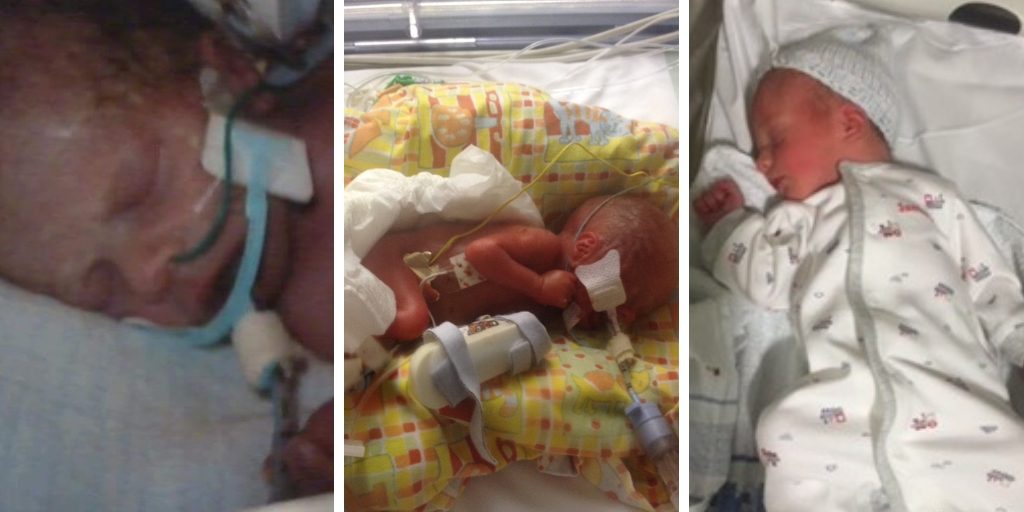
The first few moments with a new baby is a memory that all mums and dads treasure. But for parents of babies born premature or unwell, it’s a very different experience. And for the Palfey family from Cardiff, it’s something that they’ve been through more than once.
The first two trimesters of Anne’s first pregnancy had been trouble free so when she started to feel hot and swollen at around seven months, she put it down to the warm weather and a normal symptom of late pregnancy. Busy at work one afternoon, Anne almost missed the appointment that sounded the first alarm, so she will always be grateful that her midwife was happy to stay back and wait for her that day.
Noticing that Anne was quite swollen, the midwife ran tests that showed positive signs of pre-eclampsia. Anne says: “Our midwife called in a doctor to check the results and while I was in the toilet she told my husband her concerns. The doctor agreed that an ambulance should be called. But even when we got to the hospital and things started moving really quickly I wasn’t really that worried, perhaps because my mum had pre-eclampsia in pregnancy and my sister had been born prematurely , but probably because I wasn’t really aware quite what it could mean. Joe was born four hours after we arrived at the hospital. He didn’t make a sound and was immediately whisked away, but I was so full of drugs that the impact of it all didn’t really hit me until the next day.
“When the curtains went back around the cubicle on the ward the following morning, I was the only one that didn’t have my baby with me. All I had was a little picture of a son who I hadn’t even properly met yet. It ended up being a few days before I did because I was so unwell myself. I was worried that I wouldn’t recognise him and that we wouldn’t bond.”
Anne finally got to see Joe properly when he was three days old. He had suffered a bleed on his brain and had been treated for sepsis. Because his lungs were under developed he had struggled to breathe without support for the first couple days.
But despite the problems he encountered in that first week and with the help of the specialist care he received on the neonatal unit, Joe made steady progress and at five weeks old, was well enough to go home. After countless more trips to the children’s hospital for checks on his heart and general growth, doctors told Emyr and Anne that Joe was progressing as well as any other child his age.
As life returned to some semblance of normal for the Stephens family, they started to think about having a brother or sister for Joe. Sadly, despite not having had any before, Anne suffered a series of miscarriages and the couple eventually sought advice and treatment to aid a successful pregnancy. Anne became pregnant again in July 2014 and immediately began treatment to support the pregnancy.
As with Joe, the first months of Anne’s pregnancy were fine and the couple were extremely relieved that all seemed to be ok at their 20 week scan. But shortly after, Anne started to experience pains and nausea. She says: “I played it all down in my head at first. After what had happened with Joe and the miscarriages, and the worry during the first few months that I would lose this pregnancy too, I just needed it to be ok. But by the time I’d got to 24 weeks I knew something was wrong. At my next midwife appointment the baby’s growth was only measuring 21 weeks. Despite agreeing with the midwife that we would monitor things over the next few weeks, I then started noticing that the baby was moving less. By this point I was in a complete panic and we went to the assessment unit to be checked.
“I knew straight away from how the midwives were with us that they thought something was wrong too, though they tried their best to be reassuring. After a scan we were told that there may be problems with the blood flow within the placenta which was restricting the baby’s growth. The best course of action was to keep a close eye on the baby and let the pregnancy progress as far as possible while it was still ok.”
At 26 weeks however, the blood flow through Anne’s placenta started to flow in reverse and the parents were told that the safest thing for the baby now was to deliver. The neonatal team came to see them and explained that at this stage of pregnancy, the baby’s chances of survival were around 50% but that they would do everything they could to help him.
Baby Sam was delivered the next morning weighing 600 grams. He wasn’t breathing but after 15 minutes and one last attempt by the consultant, he was successfully intubated and started to receive ventilation. Anne remembers feeling like she had held her breath that whole time.
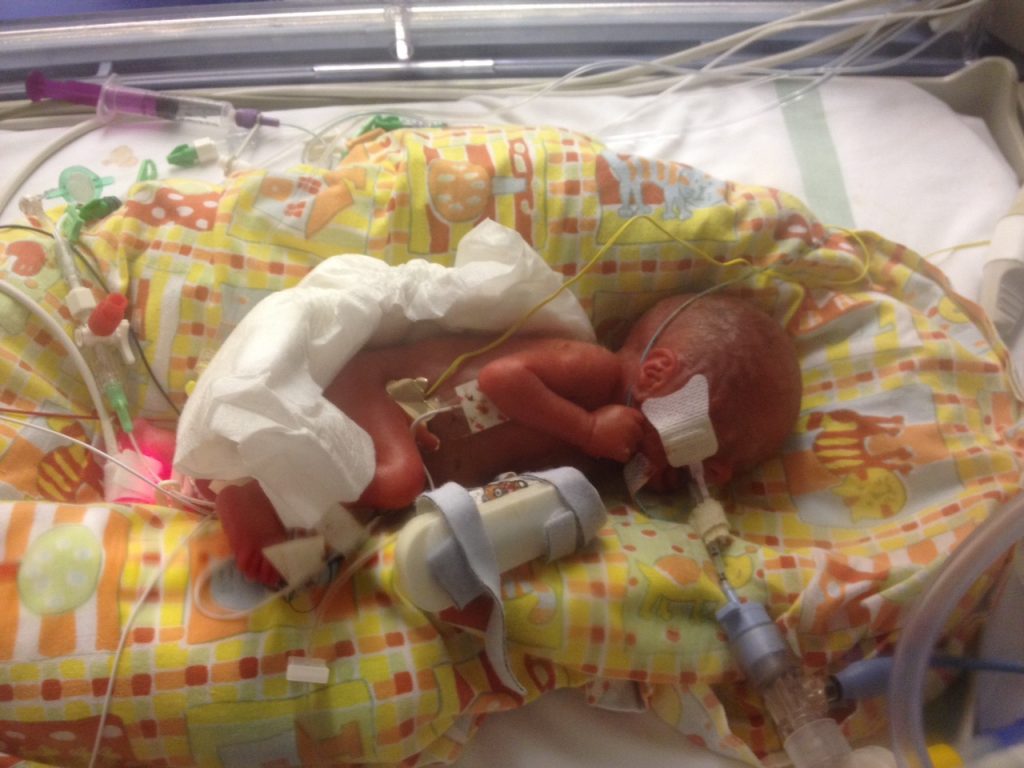
Sam was so tiny that he was put in a plastic bag to protect his skin and regulate his body temperature which babies born prematurely are unable to do. His condition was so serious that he was rushed to the intensive care unit before Anne could see him, though she says she was almost too frightened to look anyway.
Anne says: “Nothing could have prepared me for the sight of Sam in the incubator when I was finally able to see him, not even the experience we’d had with Joe. He was so small and fragile and almost completely hidden by all the tubes and machinery around him. The sight of it all was almost too much to bear but when the machines would start beeping too, I just went in to meltdown. Each time, I would think, this is it, we’re losing him.
“They’d told us that after a baby is born prematurely they often have what they call a honeymoon period, where the baby does well for a few days. Despite how frightening things were to us, that’s what seemed to happen with Sam, to the extent that our consultant told us to enjoy our Christmas with him when she left for the holiday.”
“After the first few days of relative calm, Sam developed an infection and although it was treatable, he started to struggle. Joe had come in that day to see me for the first time since Sam was born and it was then that we told him he had a brother. But while he was still with us the nurses came in to say that Sam’s condition was deteriorating rapidly and by the time we got on to the neonatal unit, there was a team around him, attempting in vain to resuscitate him. Despite the nightmare that we were witnessing I still remember noticing how upset the nurses and doctors where too. It wasn’t clinical. They were people dealing with people.”
“Losing Sam was the worst thing that ever happened to us but the nurses on the neonatal unit made sure that we had the best goodbye we could have had. We got to stay with Sam for as long as we wanted and they gave us a memory box with all his things. Despite the fact that we weren’t able to take him home, that team saved him twice, once before he was born and once just after, and they’d done everything they possibly could to save him that third time.
“Sam died on the 21st of December so Christmas was incredibly hard, particularly because we had to carry on as normal to a degree for Joe. We not only had to deal with our own feelings of grief but his too. Being so young himself he couldn’t understand why his brother hadn’t come home and for a while he was angry with me.”
Emyr and Anne were told that her placenta with Sam had contained blood clots, which can be caused by the high blood pressure she experienced in both her pregnancies. They were told that should they want to try for a baby again that with anti-clotting medication, Anne would have a 75% chance of a successful pregnancy.
Anne did fall pregnant again and was seen by her consultant, Dr Connor, every single week. Thanks to the amazing attention to detail from Dr Connor and the ante natal team, and the medication she was taking, Anne’s pregnancy progressed well up to 35 weeks, despite she says, it feeling like 35 years! At that point a scan revealed that the baby hadn’t grown for two weeks and to be entirely safe, the decision was made to deliver the baby by caesarean section. Anne and Emyr were visited once again by the neonatal team who explained that, though the pregnancy was further along than either of her previous two, the baby still may need help.
Ollie was born the same day weighing 5 and a half pound and for the very first time Anne heard her baby cry straight away. Despite needing some support to retain his temperature, she was able to keep Ollie with her and after only four days, he was well enough to go home.

Anne says: “When you have a baby it becomes the most important thing in your life and that means that without the neonatal unit there are thousands of people that wouldn’t have the most important thing in their life. That’s something that you have to deal with forever. We wouldn’t have a family at all if it wasn’t for that unit, the expensive machinery that keeps the babies alive and the amazing people who care for those babies. By fundraising we’ll always do our little bit to help make sure that all babies like Joe, Sam and Ollie get the best possible chance”.







