Eden Olive’s story

Michelle Reeves didn’t experience most of the joyful milestones associated with pregnancy and being a new mum, and many of those that she did, were a very long time coming. She didn’t get to enjoy watching her bump grow because she was scared of what might be wrong with the baby inside her and although she did look forward to meeting her new baby, she also feared for her arrival. Michelle didn’t hold her daughter until she was 12 days old and her family had to wait several months more, which made Michelle and Wesley feel that Eden-Olive was missing out on her family. Michelle wasn’t able to take her baby out for a walk in her pram until she was five months old, and she still hasn’t experienced one of the biggest milestones of all for a new mum – the journey home.
Michelle found out that she was pregnant with her first baby at 7 weeks and she, her partner Wes and step-son Jesse were overjoyed. But at 12 weeks, the family were told that their baby had tested very high risk for Downs Syndrome and this is where their problems began.
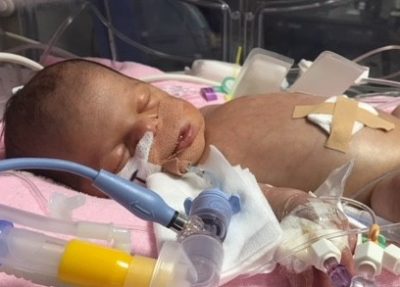
Following their 20 week scan, Michelle was referred to the foetal medicine unit after sonographers detected what they thought was an abnormality with the baby’s heart. After another scan a few weeks later, Michelle was given reassurance that the heart seemed ok, however the baby’s bones were measuring short and she underwent an amniocentesis to check for chromosomal abnormalities. Although not painful, Michelle found the process petrifying.
Michelle says: “We were on holiday in Greece when we had a phone call to say that the tests had come back negative. Wes, Jesse and I went down the water slide together in convoy to celebrate. It was the first time I’d felt completely happy in a really long time.”
But the family’s happiness was short lived. Michelle’s next visit to hospital revealed that the baby she was carrying was lacking a vascular shunt which diverts oxygenated blood from the placenta to vital organs like the liver. This meant that the baby might be born with liver damage. During the same scan, doctors also observed that the baby’s stomach was empty which was unusual. It was also empty in a follow up scan a few weeks later, and having done some research at home, Michelle asked whether her baby could be suffering from a congenital defect called oesophageal atresia, where the oesophagus doesn’t connect with the stomach. She was told that it was a possibility but there was no way of knowing for sure until the baby was born.
Michelle says: “Each time I went to the hospital I would go home in tears. I knew that the doctors were only able to tell me what they were seeing but it felt like every time I went, I was leaving with another potential problem. I loved my baby but I was petrified of her because every time I saw her on the scans I was being faced with more bad news. Pregnancy should be a happy, exciting time for a mum, but it was the most frightening thing that had ever happened to me.”
At what was to be her final scan at 35 weeks, the baby was showing signs of distress and just after 8pm that same evening, Eden-Olive was delivered by emergency C section weighing 3lb 8oz. Michelle only had time to kiss her baby’s tiny hand before she was taken away. She says: “I felt numb. I wasn’t one person with her anymore and the most important part of me had been taken away. I didn’t get to see her until late the next morning”.
An X-ray very shortly after her birth confirmed that baby Eden did have oesophageal atresia, a condition that untreated, would be incompatible with life. So, at only two days old Eden underwent a life-saving five hour operation to correct the problem. Her surgeons had to stretch her oesophagus so much to reach her stomach that Eden had to be paralysed and ventilated for the next 10 days to give her body a chance to heal. All Michelle and Wes could do was sit by her cot in intensive care and wait. They took comfort in reading her stories.

Though the operation to correct Eden-Olive’s oesophageal atresia had been a success, the procedure was a repair and not a cure and sadly the little girl’s problems didn’t end there. Michelle was delighted when she was given her first opportunity to breastfeed her baby at 13 days old, but although both took to it very well at first, within minutes Eden stopped breathing in her mum’s arms and had to be revived. Any attempt to feed her orally after that ended in the same frightening way.
After an investigative procedure to detect the cause of the problem, it was discovered that Eden also lacked an essential muscle above her stomach responsible for keep food down. As a result, she was suffering from the worst case of reflux Michelle says her doctors had ever seen and not only that, it was also causing her stomach to herniate. All attempts to feed Eden orally were stopped and instead, she received all her nutrients via a naso-jejunal tube that passed directly through her stomach and down in to her intestine.
During the weeks that followed, Michelle continued to express milk in the hope that Eden would one day be able to take it. But as time passed and Eden showed no signs of improvement, she became very despondent.
Michelle says: “The fact that I was producing all this milk but couldn’t give it to her broke my heart and still hurts now. I hadn’t been able to bath her or experience the joy of sharing her with my family but it just felt like too much of a punishment to be robbed of the most natural part of it all – to feed my baby.”
As a result of the reflux and the added discovery of a condition called tracheomalacia, which causes the airways to collapse, Michelle watched as her baby stopped breathing and needed assistance to start up again multiple times. While struggling to breathe, Eden would often pull out the tube in her nose. The procedure to replace it under X-Ray took 45 minutes and the distress that it caused Eden would affect her airways making it even harder for her to breathe. After undergoing the procedure another 15 times, the decision was finally made to replace the nasal tube with a Hickman line so that Eden could be fed intravenously, bypassing the normal digestive system.
Eden spent four and a half months on the neonatal unit before moving to Island ward at the Noah’s Ark Children’s Hospital for Wales where she now awaits an operation that is hoped will correct her problems once and for all. Michelle says that without a doubt, it’s been the most challenging year of her life, but that there are also many positive things that have come from it.
 |
“I feel very strongly that Eden was meant to be mine and that I was meant to be here to help her through this. I’ve gained friends on the neonatal unit which are friends for life and I’m so grateful to the staff both on the neonatal unit and here at Noah’s Ark for the incredible care they’ve given to my daughter. Since being here on Island ward I’ve been able to experience some of the normal things mums get to do with their babies like play in the sensory room and go outside in the garden. And the amazing play specialist Juliet has taught me so much. To have someone whose job it is to help you develop your baby despite of all the medical stuff going on is just magical. And she seems to know instinctively when I’m having a bad day and is there to give me a comforting shoulder to cry on.”
|
There’s no way I would have got through any of this without my soulmate Wes. He’s been here through the darkest of times when I know he must have been feeling scared and overwhelmed himself. My step-son Jesse who’s still only nine has been so brave too and though it must have been really hard for him not to have his dad around as much over the last eight months, he hasn’t complained once.”
At exactly nine months old, Eden went in to surgery again. Four days before the couple decided to get married, with Jesse and Eden, who would for the first time have 5 full hours away from the ward for the occasion, as their guests of honour.
“We went in to the council offices to sort out our council tax and came out with a date for our wedding! We decided to do it very suddenly but it feels like absolutely the right thing to do. We want to be a proper family unit before Eden has her big operation and by doing that it feels like we’re looking forward in to what I hope is a positive future.
“We’ve experienced such kindness from people since we made our announcement with family all rallying round to help with the wedding planning. A lovely lady called Samm Buca from Pink Butterfly Brides in Bridgend even gifted me a wedding dress and shoes and the only thing she asked in return is that I we took Eden in to see her when she finally left hospital. She asked me whether I’d been given any more gifts for the wedding and it made me think about all the endless amount of gifts that I’ve already been given. There’s the surgeons that gifted me the life of my baby and the doctors and nurses who gave the gift of care and support to Wesley and I on the most difficult days. There’s Juliet who gave me the gift of play and fun with Eden and of course there’s the gift of friendship that I’ve been given by meeting Vicky and Emma who both also have babies here at the hospital in similar situations.
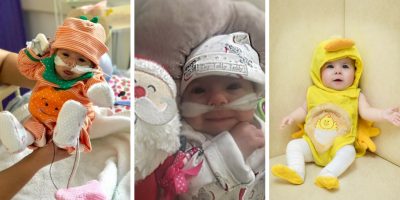
“Eden spent her first Halloween here, her first Christmas and New Year here, Mother’s Day and Easter too! I’d be lying if I said it didn’t get harder the more time passes and some days it feel so unfair. But I know there’s so much to be grateful for too and I’ll always be indebted to this hospital for saving my daughter’s life.”
The Noah’s Ark Charity support families like Eden-Olive’s by funding life-saving equipment, facilities like the sensory room and garden, and family support services like Juliet and the play specialist team.








