Edie’s story
Nicola Madoc-Jones was in work when she first noticed something was a bit different with her pregnancy. Her 20-week scan three weeks earlier had been perfect so although not too worried, Nicola and her husband David decided to go for a check just to be sure.
After various tests and examinations the couple were told that everything seemed normal, apart from one thing. Nicola was 2cm dilated, a sign that she could go in to labour at any time though there was no way of knowing when.
At only 23 weeks and 1 day pregnant, the baby’s chance of survival if delivered at that point was close to zero and would medically be classed as a late miscarriage. Each day inside the womb at that stage of pregnancy is essential and by 24 weeks the baby’s chance of survival would rise to around 50%. Although they would continue to run tests in an attempt to find a solution, in this instance it seemed like there was nothing much more they could do but wait.
The following morning, Nicola and David received a temporary glimmer of hope when told that it may be possible to put a stitch in Nicola’s cervix to delay labour. But a scan soon after revealed that, due to the positioning of the amniotic sac, it wasn’t an option in their case.
Nicola says: “Being given that little ray of hope only to have it dashed was devastating. All that was left to do now was wait and hope. Having to leave the survival of a baby to the Gods of fate felt like too much to take. One minute I’d been in the car on my way to hospital thinking about our tea and the next we were in a delivery suite talking to a consultant neonatologist. It was then the penny dropped for us. Even if our baby did survive, we’d spend months on intensive care with a very long road ahead. But, if walking down that very difficult road meant the survival of our baby, we’d take that any day.
“It felt like we were competing with the clock, watching every minute go by with my heart pounding for days. While they were doing everything they could for us, we were also being preparing us for the worst – that if I went in to labour, our baby’s chances were very slim. And the worst part was knowing that, while she was still inside me, she was healthy and well. While they were telling me that she would probably die, I could feel her moving.”
The next day, Nicola was told that as she were edging closer to 24 weeks with no further signs of labour, she would be given steroids and magnesium to mature the baby’s lungs and brain.
Nicola continues: “The relief we felt at that point was immense. We were clutching on to even the smallest bit of positive news and this meant that the doctors felt that we were approaching a point where our baby could live. We were also asked whether, if the baby was born not breathing, we wanted them to resuscitate. We said yes. I couldn’t just bring her in to the world to watch her leave.”
But only a few hours after her first course of steroids, Nicola felt something change and knew immediately that she was going in to labour. The couple were rushed to the delivery suite where they could hear their baby’s heart beating. But as soon as Nicola’s waters broke, it started to fade. Knowing that she was losing her, Nicola used all her strength to push. Baby Edie was born at 8.08am weighing 580 grams – just 23 weeks and four days in to Nicola’s pregnancy.
Nicola says: “We only got to see Edie for a few seconds before she was taken away. We were terrified to look but we couldn’t not. She was tiny, her eyes were still fused shut, her skin was translucent and she was terribly bruised from the delivery. They told us that she was extremely weak and that her odds weren’t good but just as she went, her leg moved. Amongst all the shock of the last few days, the horror of the delivery and then the tragedy that we were now expecting to unfold, that gave me the tiniest bit of hope.”
Edie was taken straight to the neonatal unit where she was put on a ventilator, given vital X-rays to assess her condition and attached to a monitor so that she could be assessed from minute to minute. The medical team also inserted lines in to her tiny veins so that she could receive medication to mature her organs and fight off infection. Although equipped to treat extreme prematurity, babies as small as Edie are rare so there were very few specific guidelines to follow for her age. The neonatal team had to think on their feet to adapt the care and equipment in order to give Edie the very best chance of life.
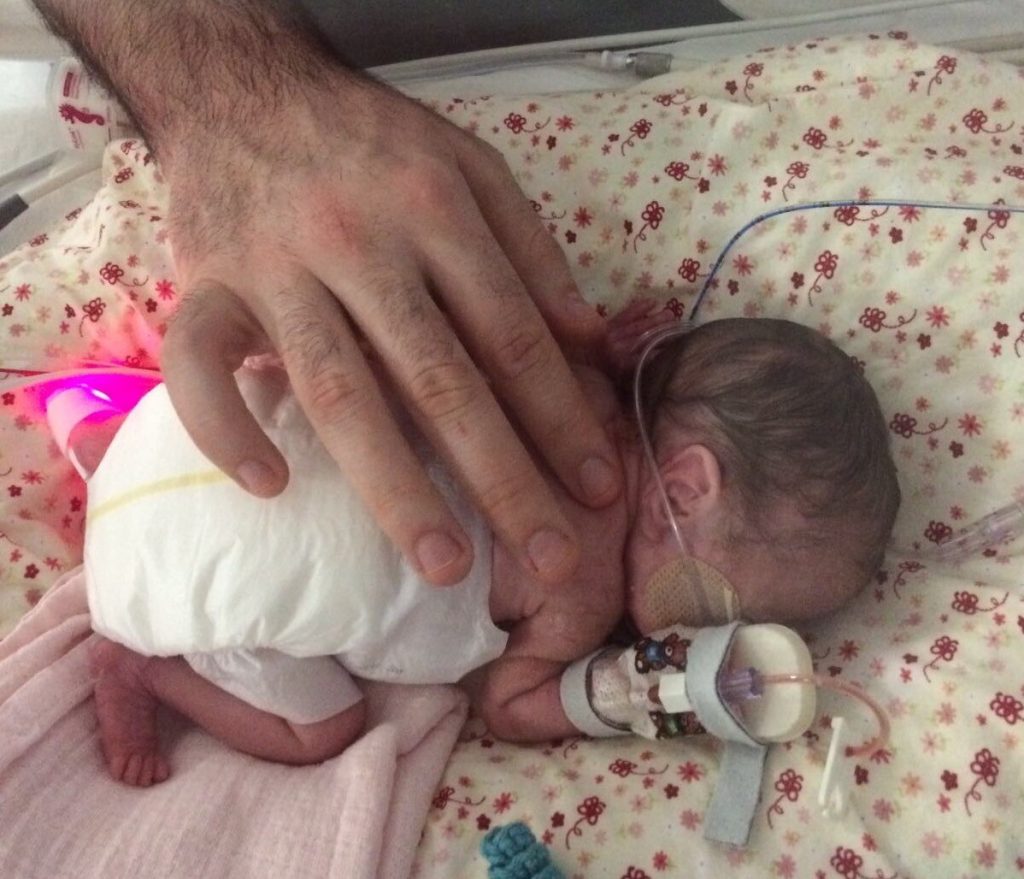
When the new parents were finally able to see Edie again, she was wrapped in a bag to keep her warm and attached to countless wires and drips. David says: “We opened the doors to this unknown world of lights, machines and alarms and lots of people dressed in blue looking after these desperately ill babies. Seeing Edie in her incubator was so far from what we’d imagined as expectant parents. What should have been so natural felt anything but and it was hard to see from looking at her how Edie would ever survive.
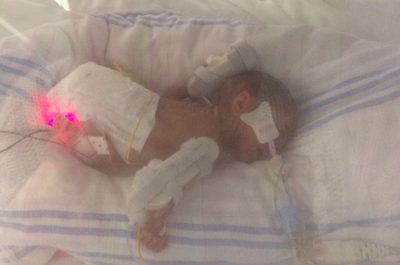
“Although we were encouraged to put our hands in to the incubator, it didn’t feel right to touch and interfere with Edie. We just wanted to leave her to grow and get strong. But for both Nicola and I, it was also a defence mechanism. If we touched her we’d always know how that felt and if we were going to lose her that just felt too painful.”
Premature babies often have what the neonatal team call a ‘honeymoon period’ in the first 24 – 48 hours after birth, where they do relatively well. Despite all the odds and a brain bleed at just a few days old, Edie’s honeymoon period lasted well in to her second week and after only five days, her lungs were working well enough to move on to a less invasive form of ventilation called BCV (Biphasic Curiass Ventilation). But Edie was so small that her body wasn’t big enough or strong enough to support even the smallest sized equipment needed to administer it, and her medical team had no option but to alternate with the ventilator.
At two weeks old, Edie developed an infection which meant that she needed the support of the ventilator full time. An X-Ray revealed that her lungs were almost filled entirely with inflammation. In order to combat her deteriorating condition, her dependency on the ventilator was increased several times. Though keeping her alive in the short term, her parents knew that the longer Edie spent on the ventilator, the less likely she was to survive. Not only was the pressure needed to keep Edie breathing also causing lung damage but the process of ventilation was also hindering her growth. Her parents were taken to a room and told by the doctors that Edie was almost at the end of the support they could provide and that once the ventilator was at full pressure, there was nothing more they could do.
Nicola says: “That was the worst day of my life. I felt sadness that was almost too overwhelming to bear. We’d spent hours sitting helplessly at Edie’s bedside, swinging between good days where nothing much happened and bad days when the alarms she was attached to rung constantly in our ears. And now we were facing the imminent prospect of leaving hospital without her, that Edie had fought all she could and her little body had nothing left. It’s every parent’s worst nightmare and we were living it. That was our reality.”
In a last attempt to get Edie off the ventilator, her doctors started to administer a course of steroids. It was a decision that bought her back from the brink and slowly over the next few weeks, Edie gained enough strength to go from the ventilator to BCV. At six weeks old she was well enough to move on to high flow – the least invasive form of ventilation. Despite the many other setbacks she faced during that time, including the need for five blood transfusions to boost her haemoglobin levels, Edie started to improve. And although Nicola and David were told that Edie may need medication with numerous scary side effects to close a dangerous hole in her heart, the hole was beginning to close unaided.
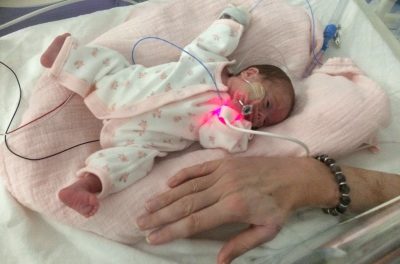
At 73 days old, Edie was moved from intensive care to the high dependency unit. At just 84 days old Edie underwent an operation to correct the growth of abnormal blood vessels in her eyes. Despite a temporary setback, she was well enough to go home with her mum and dad a short time later – a miraculous achievement for a tiny girl that not so long ago was given only the smallest chance of survival.
 |
Nicola and David are delighted at Edie’s progress and attribute it both to their amazingly resilient daughter and the incredibly skilled and resourceful neonatal team. Edie reached her official due date on the 28th of May, at 116 days old! She celebrated her actual birthday surrounded by her family and friends. Fighting fit and ready to take on the world.
|







