Baby Theo Eastment wasn’t due until the 20th of June this year so when his mum, Hayley woke up with pains on a snowy morning in March, it didn’t even occur to her that she could be in labour. At only 26 weeks pregnant, Hayley admits that she hadn’t even known it was possible to have a baby that soon.
After a few hours, the pain wasn’t going away, and as they seemed to be coming and going regularly like contractions, Hayley and Mark decided to get checked at the hospital. They were given reassurance that Hayley was probably just experiencing normal pregnancy pains but while waiting to be discharged her water’s broke. The ward staff injected Hayley with the steroids usually given to a woman in premature labour to protect the baby’s lungs and brain, but it was too late. Theo was born 20 minutes later, more than 13 weeks early and weighing a tiny 880g.
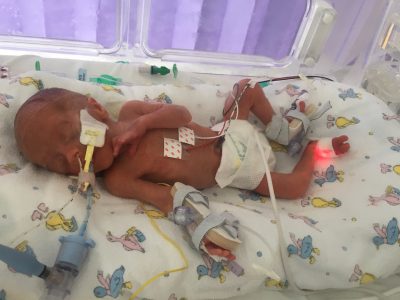
Hayley says: “I was in complete shock for those first few minutes and absolutely convinced that Theo wouldn’t be alive. I hadn’t been pregnant for long enough to go to classes or learn much about giving birth and what to expect after having a baby and there had been no time for any of the neonatal team to come and talk to us. All I had to go on were the episodes of One Born Every Minute I’d watched and from that I knew that babies usually cry when they come out. When he did give out a little cry, it gave me hope. I could only see him briefly before they took him away and I remember feeling terrified at what lay ahead of him. The thought of him feeling pain and discomfort and being apart from us was awful.”
“We were allowed to go and see Theo on the neonatal unit a few hours later and even though I was still in shock and distraught at the situation, I can remember thinking when we walked in how incredible the place was. I had no idea it existed!
“Theo looked more like a foetus than a baby when we first saw him. His skin was red and he was about the length of my forearm. His eyes were still fused shut. The nurse talked us through all the lines that were going into him and monitoring him. At this point nobody had given us any information about his chances of survival, and so we clung onto hope that there was a chance. The nurse told us that he was one of the first babies to use the brand new incubators called Baby Leo and that we could choose the colour of the light inside if we wanted to. I know it might sound silly but, as it turned out, something as small as changing the colour of the lights and having his name on the screen was the closest we got to choosing an outfit for him for a really long time.”
Hayley and Mark were told that Theo’s condition was stable and to go to get some rest. Hayley remembers them both crying together all night as the gravity of the situation hit them. She says: “I just felt so guilty. I kept thinking that it was my fault and that I must have done something wrong. I kept apologising to Mark that I hadn’t been able to keep Theo safe where he should have been. I felt like I’d failed them both.”
Theo’s condition remained stable for a few days and he started to open his eyes and move a little more. On the fourth day the medical team tried Theo on a slightly less invasive form of breathing support called BiPAP. But after only a few hours he began to struggle and he was put back on the ventilator. On the same day, Hayley and Mark were given the devastating news that a bleed on Theo’s brain which had originally been classed as low risk, was in fact a level four – the most severe grade bleed possible and that, if any swelling developed he would need emergency brain surgery. If Theo survived, it was also very likely that he would develop some form of disability as a result.
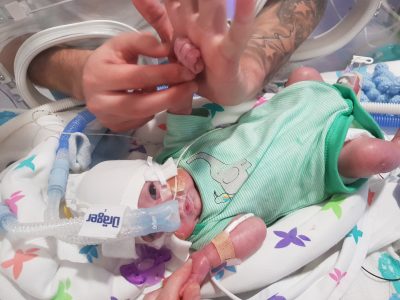
But as the hours progressed, it was Theo’s lungs that became the biggest cause for concern. Theo’s oxygen dependency increased rapidly until not even the ventilator could support his needs anymore. The only option was to transfer Theo to an oscillator – a high frequency form of ventilation that keeps the lungs permanently open. But, still, despite receiving 100% oxygen, the levels in his blood struggled to stay at 90.
Hayley says: “The doctors told us that they were extremely worried and because Theo wasn’t improving with even the highest possible type of support, the only option left was to try steroids. Most babies born early are given the best chance of survival through being given steroids and other drugs before delivery, to help the foetus mature but Theo was struggling because he didn’t get them in time. This was very frustrating for us and we were so grateful for the neonatal team for trying everything they could in a very difficult situation. We are eternally grateful for the amazing care they gave Theo and us during his stay on the unit.”
Thankfully the new course of steroids started to work and over the next week, Theo improved and on the 16th day Hayley was able to hold her son for the very first time. Mark had his first cwtch the following day but as he was still holding him, Theo’s alarms went off and his levels plummeted.
Mark says: “Don’t panic unless we panic is a common phrase used on the intensive care unit and it’s usually reassuring. But on that day, we all panicked. The whole crash team were there in seconds to intubate Theo and put him back on the ventilator again, it was clear how shaken up Theo’s nurse had been. She said that his little body had given everything in those few moments to stay alive.”
Over the next few hours Theo’s condition, despite the ventilator and steroids, continued to deteriorate. The only option left was a stronger steroid that carried a risk of further brain damage.
Mark says: “We were basically being given two options – a high risk of long term disability or death. Theo was showing so much fight and determination to be here so we had to support the neonatal team in doing everything they could. If he wasn’t giving up, neither were we.”
Theo was started on the new course of steroids and placed back on the oscillator on 100% oxygen.
Hayley says: “That night was devastating. We were in bits. We sat there for hours watching that monitor beeping, willing for his blood oxygen levels to rise, but not once did they go above 89%. In the early hours we were persuaded by the registrar to get some rest. Thankfully by the morning it was good news. Theo had started to stabilise and it seemed that the steroids had started to kick in just in time. We were so relieved, but the reality of how close he was to death has haunted us ever since”
But despite the progress Theo had made, he was by no means out of the woods. Each attempt to reduce his dose of steroids failed, he was still on intensive care 13 weeks on and Hayley and Mark were warned that if Theo’s lungs didn’t grow, within a few months there would be nothing more that could be done for him.
Hayley says: “We kept being told that he ‘just needs to grow’, but he was growing beautifully, tolerating breastmilk really well, and it was frustrating because despite him appearing to grow stronger from the outside, we knew that his lungs weren’t catching up and he was still very weak”

Just before what would have been his due date, Theo had to undergo an operation to correct a condition called ROP (Retinopathy of Prematurity) which can cause blindness in very premature babies. Despite returning to the ventilator for a short while after his eye operation, he was doing well and moved quickly down the stages of ventilation.
Mark says “Theo was getting stronger and more aware by now and he hated having the mask and prongs on his face. He constantly tried pulling them off and we sat there all day putting them back on his face so that he could have the oxygen he desperately needed. But by his due date he was stable enough to move to a nasal cannula It got to the point where he was close enough in stability to try him on High Flow, which was a nasal cannula which made him instantly more comfortable. We were so excited to see more of his face and to start seeing some progress”.
After more than 100 days on intensive care, Theo graduated to the high dependency unit. But a month later Hayley and Mark were told that an investigation to check on the severity of his reflux had uncovered a different unrelated issue. Theo had a problem with his intestine that, though nothing to do with his prematurity, was potentially lethal. He was being rushed to surgery immediately.
Hayley says: “Thankfully the operation was a success but afterwards we had to go back to intensive care. Theo had been close to death so many times while we were on that part of the unit but we’d blocked it out to move forward. Going back felt like having post-traumatic stress, hearing all the machine noises, and I found it very difficult to deal with. We were there for another week while Theo recovered from his operation and that whole time I felt sick and anxious.”
As it turned out, the operation on Theo’s intestine was more of a success than anyone could have hoped because after that, for no fathomable reason, his breathing became easier too.
At nearly six months old, and now affectionately known as the Grandad of the neonatal unit, Theo moved on to Island ward at the children’s hospital where he surprised everyone by graduating quickly on to the lowest form of ventilation called low flow. This was the best news possible for Hayley and Mark because it meant that Theo’s lungs were growing and developing – the vital information that they’ve been longing to hear.
On 20th September just over 6 months after Hayley and Mark arrived at hospital for a check, they finally got to take their baby home. But after only nine days Theo became unwell with blocked bowel caused by scar tissue from his first surgery.
Hayley says “Being back in hospital was devastating. It felt so unfair that Theo was being dealt this hand in life. All we wanted was to be at home as a family and keep him protected. We were so worried about the surgery as we knew that it would mean that Theo might have a long recovery and that he would need to go back onto the ventilator. We were worried that he might struggle to get off it, as had happened before.”
Surgery was a success and Theo was admitted to PICU on the ventilator whilst he recovered. Hayley and Mark were told that he was stable and that they would try to get him off the ventilator the following day. But for no known reason, Theo deteriorated rapidly.
Hayley says “We so were relieved that the operation had gone well and were pleased to know that we might be going home in a few days. But only 12 hours later we were told that his body was reacting very badly to something and they couldn’t understand why his lungs needed so much support”.
Two days after the surgery, at 3.30am, Hayley and Mark received the phone call telling them to go to PICU immediately.
Hayley says “We ran. We didn’t know what had happened but we know from experience that this call is never good. I was hysterical crying, running, not knowing what I would find when we got there. When we got there we saw about 20 people around Theo’s bedside performing CPR. It was the most horrific thing I have ever seen and it will haunt me for the rest of my life – seeing my baby white and lifeless knowing that he might not come back around. A doctor told us they had already been doing it for 15 minutes with no success. I pleaded for them to try everything and for Theo to come back.”
After 25 minutes Theo’s heart started beating again, but he was in a very serious condition. Hayley and Mark were told that Theo had received CPR for a very long time meaning that his brain may have been starved of oxygen and that there was a very high chance of him being brain dead.
Mark says “We had to sit next to him not knowing if he was the same boy we brought into hospital, or if he was alive at all. Every day they would turn off his paralysis for a few hours to see if he moved and responded. The first time they turned it off I kissed his ear and he moved his head away from me, which he always does, and that gave me so much hope. I just knew that he knew we were there.”
Day by day Theo made a miraculous recovery and within only 10 days he was back on low flow, awake, smiling, laughing and back to himself. It took a further two weeks to successfully wean him off all his sedation and Hayley and Mark were finally able to take their son home again on 26th October, where he continues to thrive.

Hayley says “We just can’t believe he’s still alive and we feel so lucky that he has been given this second chance at life. Theo still has severe chronic lung disease but in time, as he continues to grow, his lungs will become stronger and he will need less oxygen support. He also has issues with sickness and feeding and we know that we have a long road ahead of us with his development but we are just so grateful that he is here with us. He is such a strong boy and is doing fantastic considering his start in life. He constantly surprises us and the medical team. No matter what is thrown at him, he comes through and I just don’t know how he does it. We’ve spent over 7 months in hospital this year which has been very difficult but we find our strength in him and we are so pleased to be home”.







